After a patient receives care, a healthcare provider must complete a series of steps before getting paid.
Patient information is captured, insurance coverage is verified, approvals may be required, care is documented and coded, claims are submitted, and payments are reviewed. This process is called the healthcare revenue cycle.
In the US, it spans multiple teams, systems, and payer rules. When small breakdowns occur, payments are delayed or lost, and manual effort increases across the organization.
This project explores how AI can be used to stabilize the healthcare revenue cycle by improving accuracy, continuity, and decision-making as work moves through the system, reducing downstream rework and manual intervention.
A large share of records enter the system incomplete. Insurance rules vary by geography and payer, and change frequently. Required approvals are easy to miss. Documentation gaps often surface only after claims are submitted.
These issues are not rare edge cases. They are routine.
As a result, revenue teams spend a significant portion of their time stabilizing the process, correcting errors, and rectifying missed deadlines.
Teams repeatedly check, recheck, follow up, correct, reconcile, and resubmit. The system moves forward, but slowly and with high cognitive load.
It functions largely because people continuously intervene to keep it from breaking.
Healthcare revenue systems have not lacked software. They have lacked ownership.
Most tools support individual tasks. No tools carry context, enforce decisions, and follow work through the entire revenue cycle. As a result, teams absorb the gaps manually.
AI creates an opportunity to redesign revenue operations around continuity rather than correction.
By operating across steps instead of within silos, AI agents can turn a fragile, reactive process into a coordinated system. This shift unlocks three meaningful advantages.
Continuity across the workflow
Decisions made early in the process can carry forward, reducing information loss between handoffs.
Earlier
intervention
Issues can be identified and addressed before they compound into delays, rework, or lost revenue.
Reduced operational load
By handling repetitive verification and follow-up, AI agents free teams from constant stabilization work.
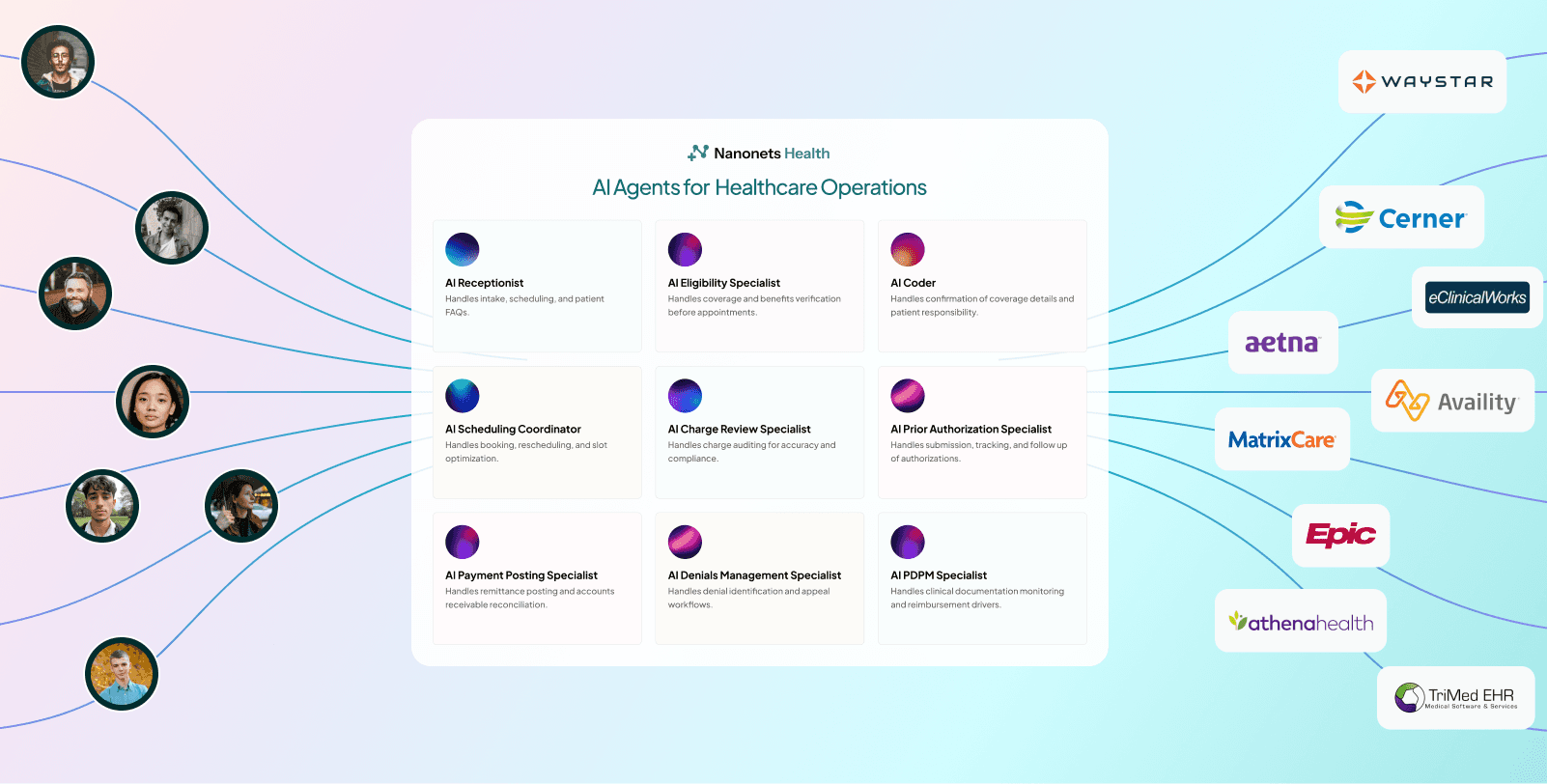
To address the lack of continuity in revenue operations, the system is designed around AI agents that operate across the entire revenue cycle.
These agents handle patient intake, verify insurance coverage before appointments, track approval requirements, interpret clinical documentation, apply billing codes, submit claims, monitor payments, and follow up on discrepancies. Context is shared across agents so decisions made early are preserved as work progresses.
By operating across steps rather than within isolated tasks, AI agents surface issues earlier, reduce gaps between handoffs, and lower the amount of manual stabilization required from teams.
The result is a revenue system that is more coordinated, more predictable, and less dependent on constant human intervention.
The purpose of this research was to build a clear understanding of how revenue operations function in practice, and to use that understanding to define what should be built, how it should work, and where Nanonets Health could meaningfully sit in the market.
This included understanding operational realities, evaluating existing tools and approaches, and identifying where current solutions fell short in supporting end-to-end revenue workflows.
Research began with interviews and workflow walkthroughs with intake teams, eligibility specialists, billing staff, and revenue leaders across U.S. healthcare organizations.
The graphic below captures the questions asked and the responses received across these conversations.
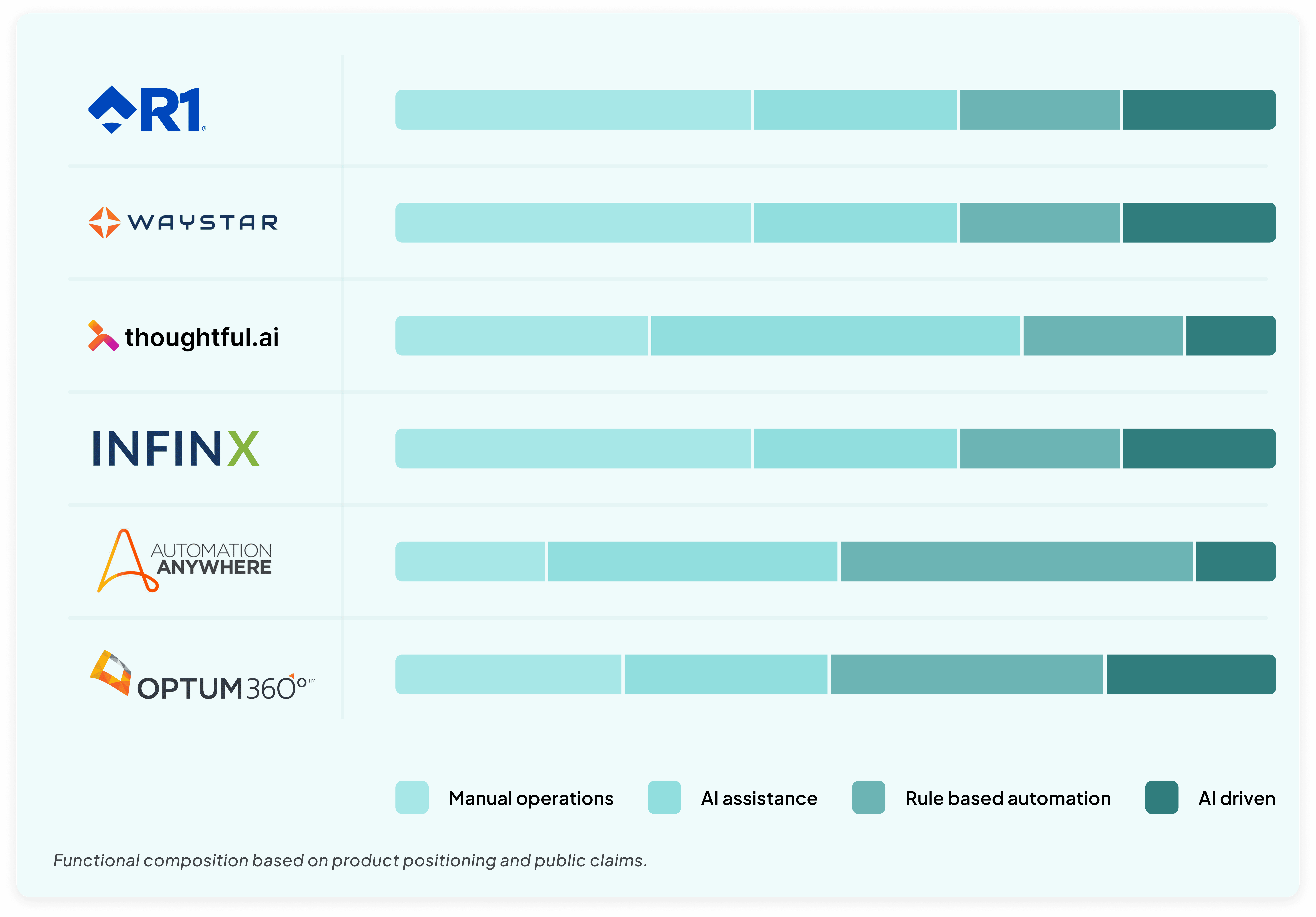
To contextualize the above findings, existing RCM platforms were reviewed across product design, workflow depth, and market positioning.
Insights from field research and market analysis were mapped together on the whiteboard.
The whiteboard reflects how manual effort filled the gaps between systems, and where responsibility repeatedly shifted back to people.
This clarified both the problem structure and the opportunity space for Nanonets Health.
With the problem space defined, early exploration focused on restructuring responsibility rather than adding features.
DESIGN LANGUAGE
Look and feel of Nanonets Health
Teal is the primary system colour, chosen for its ability to combine the trust and reliability associated with medical systems with the sense of progress and stability required for operational software. It is calming without being passive, clinical without feeling cold, and remains readable across long working sessions, helping reduce visual fatigue and signal safety without alarm.
Secondary purple is used selectively for links and moments that require light visual emphasis. All other colours are treated as subtle accents, applied sparingly to support status, variation, and clarity without drawing attention away from the core workflow.
Typography is chosen for clarity and endurance. A modern sans-serif font is used to support dense information, long review sessions, and fast scanning. Slight negative kerning is applied to create a more modern, precise, and composed visual tone while maintaining readability at scale.
Layouts are grid-based and predictable. Screens are designed to be skimmed quickly, helping users identify status, blockers, and areas requiring attention without searching or switching context.
Workflows follow consistent patterns so any AI agent can be introduced without retraining. Components behave the same across screens, making agents effectively plug-and-play within the system.
Language is factual and declarative. Copy states system status, changes, and required actions without conversational phrasing or instruction.
The logo combines the medical cross with interconnected nodes. The cross represents care, clinical responsibility, and trust. The nodes reflect Nanonets’ foundation in intelligent systems and data networks. Together, they represent AI operating within healthcare workflows in a structured and accountable way.
CORE FLOWS
How AI agents operate across the revenue cycle
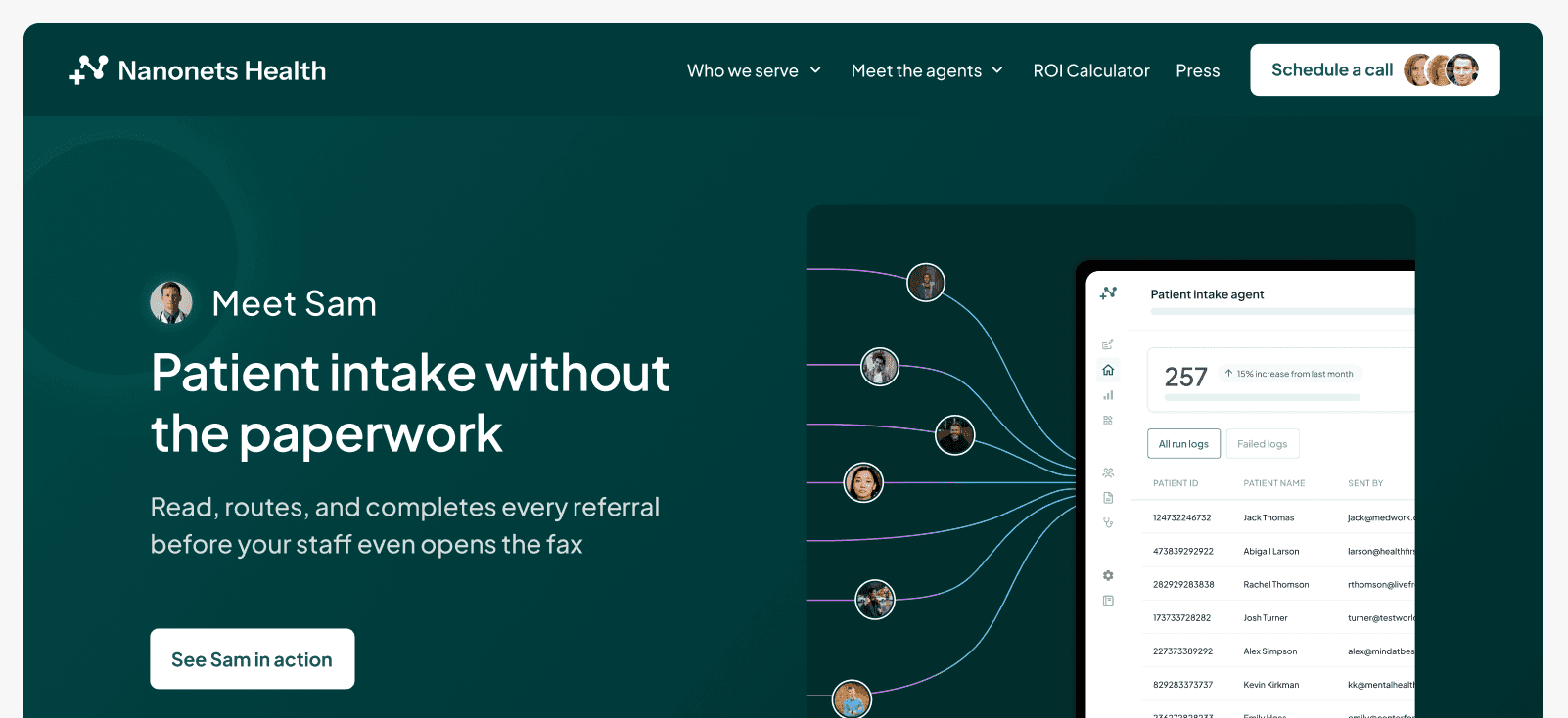
This section shows how AI agents work in practice. Each flow is illustrated through product screens that reflect how information moves, how decisions are made, and how work progresses across the system.
A single landing view where every AI agent lives. Track what is running, what is complete, current status, and where human intervention is required.
Patient page
A unified view of the patient journey. Access history, demographics, insurance details, encounters, reports, and clinical data in one place, with everything organized for review, action, and downstream workflows.
All Service Requests
The source of truth for every referral. See current status, next steps, ownership, and exceptions in one place, with clear visibility into where each request stands and what action is required next.
PDPM Agent
For SNFs to classify and reimburse care, with AI that auto-maps documentation to PDPM, flags gaps, and generates structured summaries for review and submission.
Analytics Agent
Allows users to ask questions in natural language, analyze trends, generate charts, and review performance metrics across claims and denials.
In-person conferences created opportunities to observe reactions in real time. Booth conversations and live walkthroughs surfaced where the system narrative was clear and where additional explanation was required.
Decks and collateral were used to explain workflows and outcomes, not features. These materials helped align stakeholders around how the system worked and where it fit.
Demos functioned as product tests. Walking through real workflows revealed questions, friction points, and trust gaps that did not appear in static designs.
See more product demos below:
vimeo.com
vimeo.com
vimeo.com
vimeo.com
Within the first year of deployment, Nanonets Health reached $800K in annual recurring revenue.
The product moved from early concepts to live usage across revenue teams handling real intake, eligibility, coding, and payment workflows. AI agents were operating on production data, supporting day-to-day revenue work rather than isolated pilots.